Fall 2019 (Volume 29, Number 3)
Survey on the Use of Temporal Artery Biopsy Versus Doppler Ultrasound for the Work-up of Giant Cell Arteritis
By Edsel Ing, MD, FRCSC, MPH; Qinyuan (Alis) Xu, BSc; and Philip Baer, MDCM, FRCPC, FACR
Download PDF
Abstract
To determine whether temporal artery biopsy (TABx) or doppler ultrasound (US) of the temporal artery is the preferred confirmatory test for giant cell arteritis, an online survey of rheumatologists in Ontario, Canada, was conducted in 2019. There were 71 survey respondents with an estimated survey response of 26%. Ninety percent (90%) of rheumatologists preferred TABx, 6% preferred US, and 3% used neither ultrasound nor TABx. One respondent in the latter group preferred MRI of the head.
Introduction
Temporal artery biopsy (TABx) has long been acknowledged as the “gold standard” confirmatory test in patients with suspected giant cell arteritis (GCA).1,2,3,4,5,6 However, TABx is an invasive test with potential for facial nerve palsy, hemorrhage, infection, untoward scarring and rarely stroke.
In 2018 the European League Against Rheumatism (EULAR) guidelines suggested that at centres with appropriate equipment and sufficient radiologic expertise doppler ultrasound (US) of the temporal artery or magnetic resonance imaging (MRI) may be first line investigations for suspected GCA.7 However, others do not concur.8,9,10
Materials and methods
Research ethics board approval was obtained from Michael Garron Hospital, and the research was compliant with the Declaration of Helsinki. The online survey was conducted in May and June 2019.
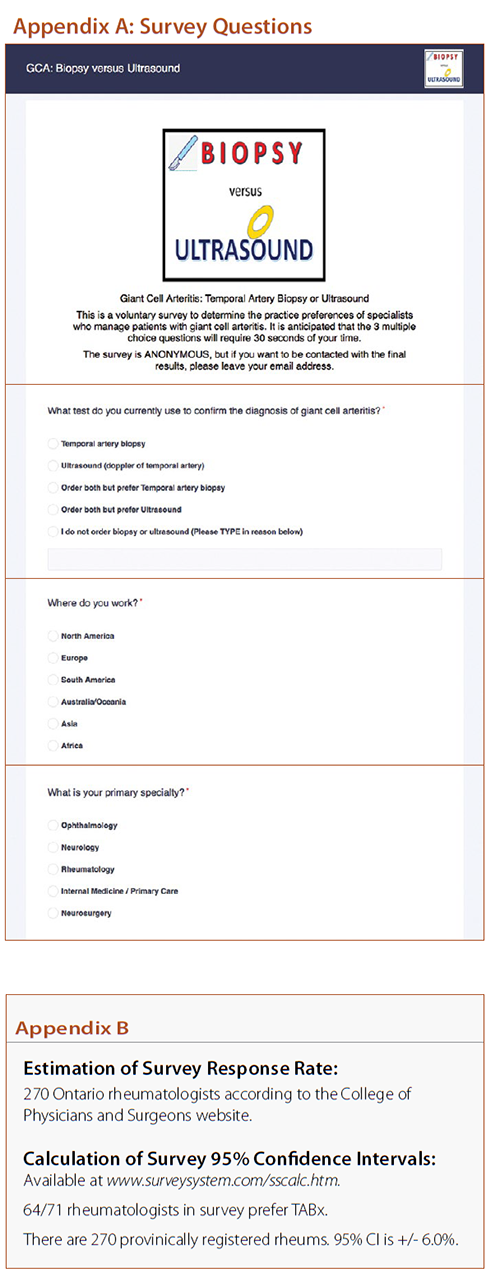
The survey instrument was Survey Planet (surveyplanet.com/sscalc.htm). The survey questions are shown in Appendix A and are available at s.surveyplanet.com/UJ2kjVmw6. The survey software prevented double entries from the same computer or internet protocol (IP) address. Rheumatologists who were members of the Ontario Rheumatology Association were targeted by a mass email and invited to participate in the survey. To maximize responses, the survey was kept anonymous and designed to be completed in 25 seconds. Respondents were allowed to freely text additional details, and their email address if they desired.
The survey margin of error (x) was determined using the calculator from www.surveysystem.com/sscalc.htm and reported as (+/- x)95% CI with the superscript denoting a 95% confidence interval.
Results
In total, 71 surveys were completed in an average time of 24 seconds +/- 15 seconds. Our estimated survey response rate was 26% (see Appendix B).
Of the 71 rheumatologists surveyed, 64 (90.1 +/- 6.0%)95% CI preferred TABx, four (5.6 +/- 4.6%)95% CI preferred doppler ultrasound, and three (4.2 +/- 3.9%)95% CI ordered neither. One rheumatologist from the latter group endorsed MRI head as his preferred investigation.
Discussion
Imaging options for the work-up of GCA include doppler ultrasound of the temporal artery +/- axillary arteries, MRI, computed tomographic imaging and positron emission tomography.
As of 2019, the majority of rheumatologists in Ontario prefer TABx to ultrasound in the work-up of GCA. EULAR guidelines notwithstanding, a systematic review comparing imaging and pathology showed that the hypoechoic halo sign on temporal artery doppler ultrasound had 68% (57%, 78%)95% CI sensitivity and 81% (75%,86%)95% CI specificity compared to a positive TABx.10 Atherosclerosis can cause false positive halo signs on doppler ultrasound.11 The low 39% sensitivity for TABx reported in the Role of Ultrasound Compared to Biopsy of Temporal Arteries in the Diagnosis and Treatment of Giant Cell Arteritis (TABUL) study12 was biased by the following: i) 7% of the TABUL biopsies did not retrieve a temporal artery, but instead structures such as veins, fat, muscle or nerve; and ii) 43% of the TABUL TABx specimens were < 1 cm; and iii) The ACR classification non-biopsy criteria were not intended for the diagnosis of GCA. The EULAR task force conceded that TABx “should be performed in all cases, where GCA cannot be confirmed or excluded based on clinical, laboratory and imaging results.”13
A potential weakness of our survey is the 26% survey response rate. However, our use of 95% confidence intervals accounts for the response rate. Furthermore, the direct correlation between response rate and study validity has been questioned.14
The results of this survey elucidate physician specialty trends in the work-up of GCA, and perhaps aid in the development of future preferred practice patterns. In the future the use of clinical prediction rules15 in conjunction with improved imaging techniques, and perhaps genetic tests may decrease the reliance on TABx.
Declaration of conflicts of interest statement
The authors report no conflicts of interest.
References:
1. Koster MJ, Warrington KJ. Giant cell arteritis: pathogenic mechanisms and new potential therapeutic targets. BMC Rheumatology 2017; 1(2).
2. Frohman L, Wong AB, Matheos K, et al. New developments in giant cell arteritis. Surv Ophthalmol. 2016; 61(4):400-21.
3. Weyand CM, Goronzy JJ. Giant-cell arteritis and polymyalgia rheumatica. N Engl J Med 2014; 371(1):50-7.
4. Ness T, Bley TA, Schmidt WA, et al. The diagnosis and treatment of giant cell arteritis. Dtsch Arztebl Int 2013; 110(21):376-86.
5. Danesh-Meyer H. Temporal artery biopsy: skip it at your patient's peril. Am J Ophthalmol 2012; 154(4): 617-9.
6. Villa-Forte A. Giant cell arteritis: suspect it, treat it promptly. Cleve Clin J Med 2011; 78(4): 265-70.
7. Dejaco C, Ramiro S, Duftner C, et al. EULAR recommendations for the use of imaging in large vessel vasculitis in clinical practice. Ann Rheum Dis 2018; 77(5): 636-43.
8. González Porto SA, Silva Díaz MT, Reguera Arias A, et al. A comparative study of doppler ultrasound against temporary artery biopsy in the diagnosis of giant cell arteritis. Reumatologia Clinica 2018; pii: S1699-258X(18)30187-6.
9. Bilyk JR, Murchison AP, Leiby BT, et al. The utility of color duplex ultrasonography in the diagnosis of giant cell arteritis: a prospective, masked study (An American Ophthalmological Society Thesis). Trans Am Ophthalmol Soc 2018; 115: T9.
10. Rinagel M, Chatelus E, Jousse-Joulin S, et al. Diagnostic performance of temporal artery ultrasound for the diagnosis of giant cell arteritis: a systematic review and meta-analysis of the literature. Autoimmun Rev 2019; 18(1): 56-61.
11. De Miguel E, Beltran LM, Monjo I, et al. Atherosclerosis as a potential pitfall in the diagnosis of giant cell arteritis. Rheumatology (Oxford) 2018; 57(2): 318-21.
12. Luqmani R, Lee E, Singh S, et al. The role of ultrasound compared to biopsy of temporal arteries in the diagnosis and treatment of giant cell arteritis (TABUL): a diagnostic accuracy and cost-effectiveness study. Health Technol Assess 2016; 20(90).
13. Moiseev SV, Smitienko I, Bulanov N, et al. The role of temporal artery biopsy in patients with giant-cell arteritis is debated. Annals of the Rheumatic Diseases 2019; 78:e3.
14. Morton SB, Bandara DK, Robinson EM, et al. In the 21st Century, what is an acceptable response rate? Aust NZ J Public Health 2012; 36(2):106-8.
15. Ing EB, Miller NR, Nguyen A, et al. Neural network and logistic regression diagnostic prediction models for giant cell arteritis: development and validation. Clin Ophthalmol 2019; 13: 421-30.
Edsel Ing, MD, FRCSC, MPH
Department of Ophthalmology and Vision Sciences,
University of Toronto
Toronto, Ontario
Qinyuan (Alis) Xu, BSc
Faculty of Medicine, University of British Columbia
Vancouver, British Columbia
Philip A. Baer, MDCM, FRCPC, FACR
Vice-President, Ontario Rheumatology Association
Past-Chair, Section of Rheumatology,
Ontario Medical Association
Scarborough, Ontario
|




